Cellular redox balance
Before we get in to the specifics of how the pentose phosphate pathway and folate/methylation cycles affect adrenal function, we need to discuss something called redox balance. Redox reactions involve the passing of electrons between molecules and are normally coupled with one another. Reduction involves a molecule gaining an electron while oxidation involves a molecule losing an electron. In order for one molecule to gain an electron, one must give up an electron, hence the pairing.You may be familiar with free radicals and antioxidants. Free radicals are molecules that have an unpaired electron in their outer shell. This makes them unstable so they "steal" electrons from other molecules. By stealing an electron, a free radical becomes more stable and is reduced while the other molecule becomes unstable and is oxidized. Antioxidants donate an electron to free radicals to prevent healthy tissues from becoming oxidized, but when they reduce free radicals they become oxidized and unstable themselves.

Based on the above information, we can call free radicals oxidizing agents and antioxidants reducing agents. Redox balance refers to the reactive state of the cell. A cell with a higher percentage of oxidizing agents will favor oxidation while a cell with a higher percentage of reducing agents will favor reduction. In addition, certain redox pairs exist in different ratios since they function as coenzymes in metabolic pathways. This is important because many biochemical reactions are dependent on cellular redox balance and this balance will dictate the direction of the pathway as each side of the coenzyme pair causes the reaction to go in a different direction.
Think of it this way. Often times, when a molecule comes to a metabolic crossroads, it encounters 2 enzymes that will direct it in opposing directions. Each one of these enzymes is dependent on a cofactor for activation. If the reduced cofactor is present in higher concentrations, the enzyme dependent on the reduced coenzyme will become active while the one dependent on the oxidized cofactor will be more dormant. This will direct the molecule down that enzymes pathway and oxidize the cofactor, increasing the chances that the next one of those molecules will go in the other direction. However, these cofactors are used in so many different reactions that it's possible to "lock" the cellular pathway to favor oxidation or reduction if the redox balance favors one or the other.
The three primary coenzyme redox pairs are FAD/FADH2, NAD+/NADH and NADP+/NADPH; noted as oxidizing agent/reducing agent. Since cells tend to maintain a very high ratio of NAD+:NADH(Approximately 700 in mammalian tissues), this coezyme pair favors oxidation while the very low NADP+:NADPH ratio in cells(.005) favors reduction. This allows cells to perform both oxidation and reduction depending on whether the enzyme in the reaction prefers NAD+/NADH as the coenzyme pair or NADP+/NADPH. In addition, some of these pairs work together as coenzymes, passing electrons between one another. FAD/FADH2 often work in concert with NADP+/NADPH as cofactors for certain enzymes, many of which are involved in adrenal function. To keep it simple, for the purposes of this blog, we will focus on NADP+/NADPH. Keep in mind, as mentioned above, that once NADPH is used in a reaction it becomes NADP+, and vice versa. We use the term redox balance because when one side of the pair goes down the other goes up.
NADPH and cellular redox balance
NADPH is a very interesting molecule. It's used in cells to provide reducing power to promote anabolic reactions as well as function as an electron donor to glutathione. Glutathione functions as the primary cellular antioxidant and exists in a reduced (GSH) and oxidized (GSSG) form. When GSH encounters a free radical, it donates an electron with the help of selenium to stabilize the free radical and becomes GSSG, its oxidized, inactive form. NADPH, in concert with riboflavin(FAD), then converts GSSG back in to the active GSH. This process converts NADPH to NADP+.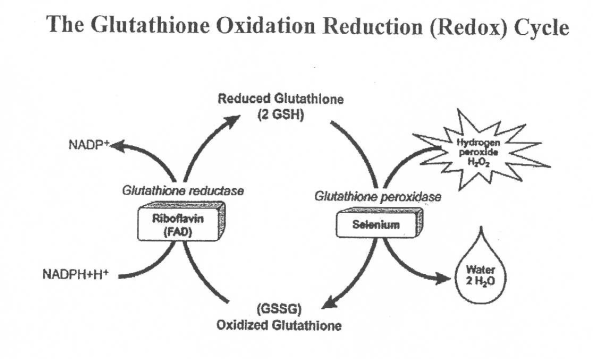

The non-oxidative phase supports this process by converting products of the oxidative phase back in to glucose 6-phosphate to create more NADPH via the enzymes transaldolase and thiamine dependent transketolase. For every molecule of glucose 6-phosphate, the pentose phosphate pathway can create 2 NADPH from NADP+ using only the oxidative phase while using both phases yields 12 NADPH provided there is enough thiamine to maintain transketolase activity. Keep in mind, when looking at redox balance, this means that the oxidative phase increases the number of NADPH by 2 and also decreases the number of NADP+ by 2 while the non-oxidative branch changes each by 12, a 24 point swing in redox balance in favor of NADPH.
Redox balance, specifically NADP+:NADPH, relates to adrenal function because biosynthesis of glucocorticoids, as well as most steroid hormonse, is dependent on NADPH(1). This could help explain why thiamine deficiency has such an impact on adrenal function because thiamine, specifically thiamine diphosphate, is necessary to get the full NADPH recharging effect of the pentose phosphate pathway. Additionally, NADP+ favors the conversion of cortisol to cortisone, a weaker glucorticoid, while NADPH favors the opposite conversion. A redox balance that favors oxidation in the adrenal glands, therefore, can have a negative impact on adrenal function by creating more cortisone than cortisol. It's interesting to note that cortisol is also capable of binding to the mineralocorticoid receptor while cortisone is not. This would negatively impact electrolyte balance by increasing sodium loss in the urine, a common casuative factor in adrenal fatigue symptoms.
While we have focused on the pentose phosphate pathway for NADPH production because it provides the greatest contribution, there are other ways NADPH can be produced. One newly discovered and very interesting pathway involves the folate cycle, so if you have an MTHFR mutation, you may want to strap in.
Next: NADPH, the folate cycle, and adrenal function